Nhổ răng và piezosurgery: kỹ thuật
A Clinical Review of Dental Extraction: Indications, Procedures, and Technological Advancements in Oral Surgery Part I: Clinical Indications for Dental Extraction: A Necessary Intervention for Oral Health While the primary objective of modern dentistry is the preservation of natural dentition, tooth extraction, or exodontia, remains a fundamental and often necessary surgical procedure. The decision to extract a tooth is never made lightly and is predicated on a thorough clinical and radiographic evaluation. Indications for extraction are diverse, ranging from advanced pathology that renders a tooth non-restorable to strategic removal for orthodontic or prosthetic purposes. In certain medical contexts, extraction serves a prophylactic role, mitigating risks to systemic health. The procedure, therefore, should not be viewed as a failure of dental care but rather as a critical therapeutic intervention aimed at eliminating pain, resolving infection, and establishing a foundation for long-term oral and systemic well-being. 1.1 Pathological Imperatives: Severe Caries and Periodontal Disease The most common drivers for dental extraction worldwide are the two most prevalent oral diseases: dental caries (tooth decay) and periodontal (gum) disease. Severe Dental Caries: Tooth decay is a progressive disease that, in its early stages, can be treated with simple restorative procedures like fillings. However, if left untreated, decay can advance through the outer enamel and dentin layers to infect the innermost pulp tissue, which contains the tooth's nerve and blood supply. At this stage, a root canal therapy can often save the tooth by removing the infected pulp. Yet, when the decay is so extensive that it has destroyed a significant portion of the tooth's structure, the tooth may become structurally compromised and non-restorable even with a crown. In such cases, extraction is the only viable option to prevent the infection from spreading to adjacent teeth, the surrounding gums, or the jawbone, a condition which can lead to a severe abscess. The removal of a severely decayed and infected tooth provides immediate relief from pain and eliminates the nidus of infection, thus reducing the harmful bacterial load in the oral cavity. Advanced Periodontal Disease: Periodontitis is a severe inflammatory condition affecting the gums and, crucially, the underlying bone that supports the teeth. In its advanced stages, the disease causes irreversible degeneration of the periodontal ligaments and alveolar bone. This loss of support leads to the loosening of teeth, a state known as tooth mobility. When bone loss is so significant that a tooth can no longer be stabilized, even with advanced periodontal treatment, extraction becomes necessary. This action prevents the tooth from eventually falling out on its own and helps protect the remaining oral structures from the ongoing disease process. 1.2 Structural and Developmental Rationale: Impaction, Crowding, and Orthodontic Strategy Beyond pathology, extractions are frequently performed to address structural and developmental issues within the dental arches. This reframes the procedure from a purely reactive measure against disease to a proactive, strategic tool used in comprehensive treatment planning. Impacted Teeth: An impacted tooth is one that has failed to fully erupt into its proper position in the dental arch and remains partially or fully submerged beneath the gum line and/or bone. This is most common with third molars, or "wisdom teeth," which are the last teeth to erupt and often find insufficient space in the jaw. Impaction can lead to a host of complications, including pain, swelling, recurrent infections (pericoronitis), and the formation of cysts or tumors. Furthermore, an impacted tooth can exert pressure on adjacent teeth, causing damage, resorption, or misalignment. Extraction of impacted teeth is therefore a preventative measure to alleviate current symptoms and avert future, more serious complications. Dental Crowding and Orthodontic Preparation: In cases where a patient's jaw is too small to accommodate all of the permanent teeth, severe crowding can occur. This misalignment can impair function, compromise oral hygiene, and be aesthetically displeasing. As part of a comprehensive orthodontic treatment plan, one or more teeth may be strategically extracted to create the necessary space for the remaining teeth to be moved into proper alignment with braces. This type of extraction is most frequently performed on children and teenagers undergoing orthodontic correction and is a clear example of extraction being used not to treat disease, but to facilitate an ideal functional and aesthetic outcome for the entire dentition. 1.3 Traumatic Injuries and Non-Restorable Fractures Dental trauma resulting from accidents, falls, or sports injuries can cause teeth to fracture or break. While many fractures can be repaired with bonding, crowns, or other restorative techniques, some are too severe to be salvaged. A tooth that is fractured at or below the gum line often does not leave enough sound tooth structure exposed to support a crown, rendering it non-restorable. Such fractures can also create a pathway for bacteria to infect the pulp and surrounding bone. In these acute situations, extraction is often the only course of action to prevent pain and infection. In some cases of dental trauma, an extraction may be required as an emergency procedure. 1.4 Prophylactic Extractions in Medically Compromised Patients A particularly sophisticated application of dental extraction lies in the management of medically compromised patients. For individuals with severely weakened immune systems—such as those undergoing chemotherapy, preparing for an organ transplant, or receiving certain other medical treatments—a dental infection can pose a significant, even life-threatening, risk. In these contexts, a tooth that has a questionable long-term prognosis, even if it is currently asymptomatic, may be recommended for prophylactic extraction. This proactive approach removes a potential source of future infection, thereby preventing severe systemic health complications in a patient who is ill-equipped to fight them. This demonstrates a critical integration of dental and medical care, where the decision to extract is driven by a holistic assessment of the patient's overall health and the potential for a localized oral issue to escalate into a systemic crisis. This elevates the role of exodontia from a tooth-centric procedure to an integral component of comprehensive patient health management. Part II: The Dental Extraction Procedure: A Comprehensive Clinical Overview The clinical process of a dental extraction is a meticulously planned procedure that begins with a thorough diagnostic phase and culminates in the removal of the tooth. The specific technique employed is dictated by the tooth's condition, position, and accessibility. The distinction between a "simple" and a "surgical" extraction is not merely descriptive but is a fundamental classification that determines the entire clinical pathway, influencing the choice of practitioner, the required level of anesthesia, the procedural cost, the patient's recovery trajectory, and the likelihood of specific complications. 2.1 Patient Evaluation and Radiographic Assessment Prior to any extraction, a comprehensive evaluation is mandatory. This begins with a physical assessment of the tooth and surrounding tissues by the dentist. However, a visual examination alone is insufficient. Radiographic imaging, typically in the form of dental X-rays, is essential for a complete diagnosis and for procedural planning. X-rays provide critical information about the structures below the gum line, revealing the length, shape, and curvature of the tooth's roots. They can also identify hidden pathologies such as root fractures, bone infections, or the proximity of the tooth to vital anatomical structures like nerves and sinuses. This detailed anatomical information allows the clinician to anticipate potential difficulties and determine the most appropriate and safest method for removal, forming the basis for the decision to perform either a simple or a surgical extraction. 2.2 Simple Extraction: Technique and Instrumentation A simple extraction is indicated for a tooth that is fully erupted, visible in the mouth, and can be accessed without complex surgical intervention. This procedure is commonly performed by general dentists in an outpatient setting under local anesthesia. The process begins with the administration of a local anesthetic to numb the tooth, gum, and surrounding bone tissue. Once the area is profoundly numb, the dentist uses a specialized instrument called a dental elevator. The elevator is carefully inserted between the tooth and the bone of the socket to sever the periodontal ligament, which holds the tooth in place. By applying controlled pressure and twisting motions, the dentist uses the elevator to gently rock the tooth back and forth, expanding the socket and progressively loosening the tooth. Once the tooth is sufficiently mobile, dental forceps are used. These are plier-like instruments designed to firmly grasp the visible crown of the tooth. The dentist then applies steady, controlled pressure to continue rocking the tooth and ultimately remove it from the socket. Throughout this process, the patient should not feel any sharp pain due to the anesthetic, but sensations of pressure are normal and expected. 2.3 Surgical Extraction: Flap Design, Bone Removal, and Tooth Sectioning A surgical extraction is a more complex and invasive procedure required when a tooth cannot be easily accessed. This includes teeth that are impacted (not fully erupted), have broken off at the gum line, or have long, curved roots that prevent a simple removal. While some general dentists perform surgical extractions, complex cases are often referred to an oral and maxillofacial surgeon. The procedure necessitates surgical access to the tooth. After anesthesia is administered, the surgeon uses a scalpel to make a precise incision in the gum tissue near the tooth. This allows the surgeon to create and lift a section of the gum tissue, known as a mucoperiosteal flap, away from the underlying bone. This step exposes the bone that encases the tooth root. In many cases, some of the bone overlying the tooth must be removed to gain access to the root or to create a path for its removal. This is typically done using a high-speed surgical drill or bur with copious water irrigation to prevent overheating and damage to the bone. For multi-rooted teeth, such as molars, or for teeth that are firmly lodged, the surgeon may need to section the tooth. This involves using the surgical drill to cut the tooth into smaller, more manageable pieces, which can then be removed one at a time. This technique is often less traumatic than attempting to remove a large, complex tooth in one piece. Once all pieces of the tooth have been removed, the surgeon may clean the socket, smooth any sharp edges of bone, and reposition the gum flap. The incision is then typically closed with sutures (stitches) to facilitate healing. The increased complexity, tissue manipulation, and potential for bone removal inherent in a surgical extraction mean that it is associated with a longer recovery period, greater post-operative discomfort, and a higher risk of complications compared to a simple extraction. Part III: Anesthesia and Sedation in Oral Surgery: A Patient-Centric Approach to Pain and Anxiety Management The management of pain and anxiety is a cornerstone of modern oral surgery. The evolution of anesthetic and sedative techniques reflects a sophisticated understanding that patient comfort is paramount and that psychological distress can be as significant a barrier to care as physical pain. The contemporary spectrum of options ranges from localized numbing to complete unconsciousness, allowing for a tailored approach that considers both the clinical complexity of the procedure and the individual patient's level of apprehension. This creates a dual-axis decision-making model where the choice of anesthesia is guided not only by the surgical requirements but also by the patient's psychological needs. A patient with extreme dental phobia, for example, may be offered a deeper level of sedation for a clinically simple procedure, a choice driven entirely by the need to manage their anxiety. 3.1 Pharmacology of Local Anesthesia Local anesthesia is the foundation of pain control for nearly all dental extractions. It involves the administration of a numbing agent, such as lidocaine, via injection directly into the soft tissues surrounding the target tooth. The anesthetic solution works by temporarily blocking the nerve pathways that transmit pain signals from the surgical site to the brain. This results in a profound state of numbness in a localized area, ensuring the patient does not feel pain during the procedure. While pain is eliminated, the nerves that transmit the sensation of pressure are not affected, so patients will typically feel the movements and pressure associated with the extraction. Local anesthesia is used in all oral surgery procedures, either alone for simple extractions or in combination with other forms of sedation for more complex cases or anxious patients. The effects are temporary, typically wearing off within a few hours following the procedure. 3.2 Conscious Sedation Modalities: A Spectrum of Relaxation For patients who experience anxiety or fear related to dental procedures, or for those undergoing longer or more complex surgeries, conscious sedation can be employed in addition to local anesthesia. These methods are designed to induce a state of deep relaxation while allowing the patient to remain conscious and able to respond to commands.
- Nitrous Oxide ("Laughing Gas"): This is a mild sedative gas mixed with oxygen that is inhaled through a small mask placed over the nose. It induces a feeling of relaxation and well-being, effectively reducing anxiety. The patient remains fully conscious and in control of their bodily functions. A major advantage of nitrous oxide is its rapid onset and quick recovery; the effects wear off within minutes of the mask being removed, allowing patients to drive themselves home.
- Oral Sedation: This method involves the patient taking a prescribed sedative pill, typically from the benzodiazepine class (e.g., diazepam), about an hour before the procedure. It produces a deeper level of sedation than nitrous oxide, significantly reducing anxiety and often creating an amnesic effect where the patient has little to no memory of the surgery. Due to the lingering effects of the medication, patients undergoing oral sedation must arrange for an escort to drive them to and from their appointment.
- Intravenous (IV) Sedation ("Twilight Sedation"): This is a more profound form of conscious sedation where sedative drugs are administered directly into the bloodstream through an IV line. This method allows for a rapid onset of sedation and gives the clinician precise control over the level of sedation throughout the procedure, titrating the medication to the patient's needs. Patients enter a state of deep relaxation, often described as a "twilight sleep," where they may drift in and out of consciousness but are comfortable and calm. This technique typically results in significant amnesia of the procedure. As with oral sedation, an escort is mandatory.
3.3 General Anesthesia: Complete Unconsciousness General anesthesia represents the deepest level of sedation, inducing a controlled state of complete unconsciousness where the patient is asleep and entirely unaware of the surgical procedure. This is typically reserved for the most intensive and complex oral surgeries, such as the removal of deeply impacted wisdom teeth or extensive implant placement. However, it is also an option for patients with extreme dental phobia or certain medical conditions, regardless of the procedure's complexity. When under general anesthesia, the patient's vital signs, including heart rate, blood pressure, and oxygen levels, are closely and continuously monitored by a trained and certified oral and maxillofacial surgeon or anesthesiologist to ensure safety. Recovery from general anesthesia is longer, and patients require a responsible adult to drive them home and monitor them for the remainder of the day. Table 1: Comparison of Anesthesia and Sedation Modalities Modality Level of Consciousness Administration Method Key Benefits Key Considerations Ideal Patient Profile Local Anesthesia Fully awake and conscious Injection into gum tissue Effective pain control at the surgical site; quick recovery Does not reduce anxiety; patient feels pressure All patients undergoing extraction, used alone for calm patients during simple procedures Nitrous Oxide Conscious, relaxed, responsive Inhalation via nasal mask Mild anxiety relief; rapid onset and recovery; patient can drive home Not suitable for patients with certain respiratory conditions or severe anxiety Patients with mild to moderate dental anxiety undergoing simple or moderately complex procedures Oral Sedation Conscious but drowsy; may have limited memory Oral pill taken pre-procedure Significant anxiety reduction; non-invasive administration; amnesic effect Sedation level is not easily adjusted; requires an escort; lingering drowsiness Patients with moderate anxiety who prefer not to have an IV line IV Sedation Deeply relaxed ("twilight sleep"); may drift in and out of sleep Intravenous line in arm or hand Rapid onset; controllable sedation level; profound relaxation and amnesia Requires an IV insertion; requires fasting and an escort; more costly Patients with moderate to severe anxiety or those undergoing longer, more complex surgical procedures General Anesthesia Completely unconscious and unaware Intravenous line and/or inhaled agents Complete elimination of pain, anxiety, and awareness; ideal for complex surgery Highest level of risk; requires close monitoring; longer recovery; requires fasting and an escort Patients with extreme dental phobia or undergoing highly invasive/lengthy oral surgeries Part IV: Post-Operative Management and Recovery Protocol Successful recovery from a dental extraction is not merely a passive process of waiting for time to pass; it is an active phase of care in which the patient plays a critical role. The post-operative instructions provided by the clinician are not arbitrary rules but are a carefully designed protocol based on physiological principles of wound healing. Adherence to this protocol is paramount for minimizing complications and ensuring a smooth, comfortable recovery. The central objective of nearly every instruction is the protection of the blood clot that forms in the tooth socket, as this fragile biological structure is the cornerstone of the entire healing process. 4.1 The Critical First 48 Hours: Hemostasis and Clot Preservation The immediate post-operative period is focused on achieving hemostasis (stopping the bleeding) and fostering the formation and preservation of a stable blood clot within the empty socket. This blood clot serves two vital functions: it protects the exposed underlying bone and nerve endings from the oral environment, and it acts as a scaffold for the new tissue that will eventually fill the space. To facilitate this, patients are instructed to bite down with firm, steady pressure on a folded piece of sterile gauze placed over the extraction site for at least 30 to 60 minutes after the procedure. This pressure helps to control bleeding and encourages clot formation. The gauze may need to be changed every 20-45 minutes if bleeding continues. During the first 24 to 48 hours, the most critical instruction is to avoid any activity that could create negative pressure or suction in the mouth, as this can easily dislodge the delicate clot. Prohibited activities include:
- Using a drinking straw
- Spitting forcefully
- Vigorous rinsing
- Smoking, as the act of inhaling creates suction and the chemicals in tobacco can impair healing
Additionally, patients should limit strenuous physical activity and keep their head elevated with pillows, even while sleeping, to help minimize bleeding and swelling. 4.2 Managing Pain, Swelling (Edema), and Bruising (Ecchymosis) A certain degree of pain, swelling, and bruising is a normal inflammatory response to surgery. Proactive management of these symptoms can significantly improve patient comfort.
- Pain Management: Post-operative discomfort typically begins as the local anesthetic wears off. It is often recommended that patients take their first dose of pain reliever before the numbness completely subsides. For most extractions, over-the-counter non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen are effective. For more complex surgical extractions, a stronger prescription pain medication may be provided. These medications should be taken as directed to control discomfort, but they may not eliminate it entirely.
- Swelling and Bruising: Swelling is the body's natural response to tissue manipulation and typically reaches its peak 48 to 72 hours after the surgery before beginning to subside. To minimize swelling, patients should apply ice packs to the outside of the face over the surgical area. An intermittent application schedule—20 minutes on, followed by 20 minutes off—is most effective and should be continued throughout the first day. After the first 24-48 hours, the application of moist heat (such as a warm, damp towel) can help reduce any residual swelling, soothe sore jaw muscles, and alleviate stiffness.
4.3 Dietary Progression and Oral Hygiene Modifications Proper nutrition and hygiene are essential for healing, but modifications are required to protect the surgical site.
- Diet: For the first few days post-extraction, a soft food diet is necessary to avoid disturbing the socket. Recommended foods include soups, yogurt, ice cream, mashed potatoes, scrambled eggs, and milkshakes. Patients should avoid thermally hot foods and beverages on the day of surgery, as heat can promote bleeding. It is also crucial to avoid hard, crunchy, or sharp-edged foods (e.g., chips, nuts, seeds, popcorn) for at least a week, as these particles can become lodged in the socket and cause irritation or infection.
- Oral Hygiene: Maintaining a clean mouth is vital to prevent infection. However, the surgical site must be treated gently. Patients can typically resume brushing their teeth on the evening of surgery or the following day, but they should be very careful to avoid the extraction site itself. As noted, vigorous rinsing and spitting are forbidden for the first 24 hours. After this period, gentle rinsing with a warm salt water solution (1/2 teaspoon of salt in a glass of warm water) two to three times a day can help keep the area clean and promote healing.
Table 2: Post-Operative Care Protocol: A Patient Guide Timeframe Key Objective Recommended Actions (Do's) Prohibited Actions (Don'ts) First Hour Achieve Hemostasis & Clot Formation Bite firmly and continuously on gauze. Rest and limit activity. Do not spit, rinse, drink, or remove the gauze. First 24 Hours Protect the Blood Clot Keep head elevated. Apply ice packs intermittently (20 min on/20 min off). Eat only soft, cool foods. Take pain medication as directed. Do not smoke, use a straw, spit forcefully, or rinse vigorously. Avoid alcohol and strenuous activity. Do not consume hot liquids. Days 2-3 Post-Op Manage Inflammation & Promote Healing Continue soft food diet. Begin gentle warm salt water rinses after 24 hours. Apply moist heat to manage swelling and jaw stiffness. Continue to avoid smoking, using straws, and hard/crunchy foods. Do not disturb the socket with tongue or fingers. First Week Maintain Hygiene & Gradual Return to Normal Function Continue gentle salt water rinses. Brush teeth gently, carefully cleaning near the surgical site. Gradually reintroduce more solid foods as comfort allows. Avoid sharp or hard foods (e.g., chips, seeds, popcorn) that could get stuck in the socket. Part V: Navigating Potential Complications in Post-Extraction Healing While the majority of dental extractions heal without incident, particularly when post-operative instructions are followed diligently, potential complications can arise. These can range from the common and painful condition of alveolar osteitis to less frequent but more serious issues such as infection and nerve damage. A significant portion of these adverse outcomes are directly linked to either the intrinsic difficulty of the procedure or the patient's post-operative actions, creating a shared-responsibility model where both clinician skill and patient compliance are critical determinants of a successful outcome. 5.1 Alveolar Osteitis ("Dry Socket"): Etiology, Risk Factors, and Management Alveolar osteitis, commonly known as "dry socket," is the most frequent complication following a tooth extraction. It is a painful condition that occurs when the blood clot that should form in the socket is either dislodged, dissolves prematurely, or fails to form in the first place. The loss of this clot leaves the underlying alveolar bone and nerve endings exposed to the oral environment, including air, food, and fluids.
- Symptoms: The hallmark symptom of a dry socket is severe, persistent, throbbing pain that typically begins one to five days after the extraction, often worsening from the initial post-operative discomfort. The pain is localized to the socket but frequently radiates to the ear, eye, or temple on the same side of the face. Other signs include a foul odor or unpleasant taste emanating from the mouth (halitosis) and a visible empty socket where the dark blood clot should be.
- Risk Factors: The development of dry socket is associated with several factors that compromise clot formation or stability. These include:
- Smoking and Tobacco Use: The chemicals in tobacco can impair healing, and the physical act of sucking on a cigarette can dislodge the clot.
- Improper At-Home Care: Failure to follow post-operative instructions, such as using a straw or spitting forcefully, directly increases the risk.
- Difficult or Traumatic Extractions: More complex surgical extractions, especially of impacted lower wisdom teeth, are associated with a higher incidence of dry socket due to the increased tissue manipulation.
- Oral Contraceptives: High estrogen levels from birth control pills may interfere with normal healing processes and increase risk.
- Pre-existing Infection: A history of infection in or around the tooth being extracted can also predispose a patient to dry socket.
- Management: A dry socket requires professional intervention. The dentist or oral surgeon will gently flush the socket to remove any food debris and then place a medicated dressing inside. This dressing contains agents that soothe the exposed bone and promote healing, providing significant pain relief. The dressing may need to be changed every few days until the socket begins to heal and the pain subsides.
5.2 Infection, Paresthesia (Nerve Damage), and Sinus Communication While less common than dry socket, other complications can occur, particularly following surgical extractions.
- Infection: Although preventative measures are taken, bacteria can sometimes enter the extraction site and cause an infection. Signs of infection include an increase in swelling or pain after the first 72 hours, persistent fever, a foul-tasting discharge from the socket, and swollen lymph nodes. If an infection develops, it is typically treated with a course of antibiotics prescribed by the clinician.
- Nerve Damage (Paresthesia): This is a rare but serious complication that can occur when a tooth, most often a lower wisdom tooth, is located in close proximity to a major nerve, such as the inferior alveolar nerve. During a surgical extraction, this nerve can be bruised or damaged. Symptoms include persistent numbness, tingling, or a burning sensation in the tongue, lip, or chin on the affected side. While this nerve damage is often temporary and resolves over weeks or months, in some rare instances, it can be long-lasting or permanent.
- Sinus Communication: The roots of the upper molars and premolars are often situated very close to the maxillary sinus cavity. During the extraction of one of these teeth, a small opening (communication) can be created between the mouth and the sinus. Small communications often heal on their own, but larger ones may require a subsequent surgical procedure to close the opening and prevent sinus complications.
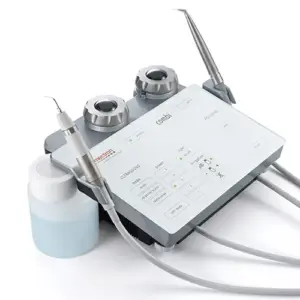
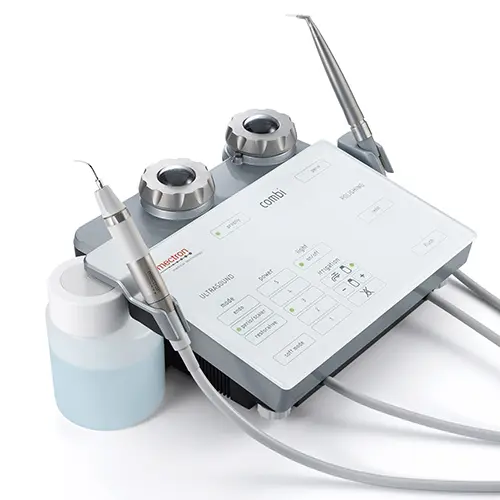
Part VI: Piezosurgery: An In-Depth Analysis of Ultrasonic Technology in Modern Extractions In the ongoing pursuit of less invasive and more precise surgical techniques, the field of oral and maxillofacial surgery has seen the introduction of advanced technologies designed to improve patient outcomes. Among the most significant of these is Piezosurgery, a technique that utilizes ultrasonic vibrations for osteotomy (bone cutting). This technology represents a fundamental paradigm shift, moving away from the macro-mechanical friction of traditional rotary instruments like drills and burs toward a more sophisticated method based on controlled, selective micro-vibrational energy. This physical distinction is the root cause of its primary clinical advantages, particularly its ability to selectively act on hard tissues while preserving adjacent soft tissues. 6.1 The Physics of Piezoelectricity: From Principle to Clinical Application The scientific principle underlying Piezosurgery is the piezoelectric effect, a phenomenon first described by physicists Jacques and Pierre Curie in 1880. The term "piezo" is derived from the Greek word piezein, meaning "to squeeze" or "press". The Curies discovered that when mechanical pressure is applied to certain crystalline materials (like quartz) or ceramics, they generate an electrical potential. Conversely, when an electric field is applied to these same materials, they undergo a physical deformation, or change in shape. This "reverse piezoelectric effect" is harnessed in modern Piezosurgery devices. The surgical handpiece contains piezo-ceramic rings. When an electric current from a generator is passed through these rings, they deform and reform rapidly, creating high-frequency microvibrations. These vibrations are then transmitted to a specialized metal tip, or insert, at the end of the handpiece, which becomes the cutting instrument. 6.2 Mechanism of Action: Selective Micrometric Cutting and Cavitation Effect The innovation of Piezosurgery lies not just in the use of vibrations, but in the precise control of their frequency. The devices are calibrated to produce ultrasonic vibrations typically in the range of 24–36 kHz. This specific frequency range is highly effective at cutting mineralized, hard tissues like bone and teeth. The critical advantage of this mechanism is its selective cutting capability. While the microvibrations efficiently cut rigid, crystalline structures, they are not effectively transferred to elastic soft tissues like nerves, blood vessels, and sinus membranes. When the vibrating tip comes into contact with soft tissue, the tissue tends to oscillate with the tip rather than being lacerated. This intrinsic property makes the technology exceptionally safe, as it minimizes the risk of accidental damage to vital anatomical structures that are often in close proximity to the surgical site. This stands in stark contrast to traditional rotary drills and burs, which are non-selective and will cut any tissue they contact, hard or soft. Furthermore, the ultrasonic vibrations, combined with a simultaneous irrigation of sterile saline solution, create a phenomenon known as the cavitation effect. This process generates vapor bubbles that expand and collapse, producing micro-shockwaves. This effect helps to create a clean, virtually bloodless surgical field by disrupting small blood vessels and washing away debris, which significantly improves the surgeon's visibility during the procedure. 6.3 Clinical Applications Beyond Extraction While Piezosurgery has gained significant favor for its application in complex tooth extractions, its versatility has led to its adoption across a wide range of oral and maxillofacial surgical procedures. The precision and safety of the technology make it an ideal tool for delicate operations involving bone. Its applications include:
- Sinus Lift Procedures: Elevating the maxillary sinus membrane for bone grafting, where the risk of perforating the delicate membrane is a primary concern with traditional instruments.
- Bone Grafting: Harvesting blocks of bone from one site to be placed in another, or preparing a site to receive graft material.
- Implant Site Preparation: Creating the precise osteotomy for dental implant placement, especially in areas with limited bone or proximity to nerves.
- Ridge Expansion and Bone Splitting: Widening a narrow jawbone ridge to accommodate an implant, a procedure that carries a risk of fracture with conventional tools.
- Crown Lengthening: Removing small amounts of bone around a tooth to expose more structure for a crown.
- Cystectomy: The removal of cysts from the jawbone or sinuses without damaging surrounding soft tissues.
The broad utility of Piezosurgery underscores its value as a significant technological advancement in the field, offering a safer and more refined alternative for numerous bone-related surgical interventions. Part VII: Comparative Analysis: Piezosurgery vs. Conventional Extraction Techniques The adoption of Piezosurgery into clinical practice prompts a critical comparison with conventional extraction methods, which primarily rely on manual elevators and forceps for simple extractions, and high-speed rotary instruments (drills and burs) for surgical ones. The analysis reveals a fundamental clinical trade-off: conventional methods often offer greater speed and efficiency, while Piezosurgery provides a range of significant benefits related to patient comfort, safety, and the quality of healing. The optimal choice is therefore not absolute but depends on the specific clinical scenario, the anatomical risks involved, and the priorities of both the clinician and the patient. 7.1 Surgical Time and Clinical Efficiency A consistent finding in the clinical literature is that Piezosurgery is a slower bone-cutting technique compared to traditional rotary instruments. The micrometric, precise nature of the cutting action inherently requires more time to remove the same volume of bone as a high-speed drill. This increased chairside duration is often cited as a primary limitation of the technology and can be a practical drawback in a high-volume clinical setting. While some local dental clinics in Vietnam market the technology as shortening extraction time, these claims may be context-dependent (e.g., for specific wisdom tooth cases) or may not reflect the broader evidence from systematic reviews, which point to longer surgical times. 7.2 Patient-Reported Outcomes: Pain, Swelling, and Trismus The most pronounced and well-documented advantage of Piezosurgery lies in the significant improvement of the post-operative patient experience. The less traumatic nature of the procedure directly translates into a milder inflammatory response.
- Reduced Pain: Multiple studies and a systematic review conclude that patients who undergo extractions with Piezosurgery report significantly less post-operative pain compared to those treated with conventional drills. Most patients experience minimal discomfort after the procedure.
- Reduced Swelling and Trismus: Piezosurgery also leads to a marked reduction in post-operative swelling (edema) and trismus (restricted jaw opening or "lockjaw"). The minimal invasiveness and reduced tissue trauma result in a more comfortable recovery period.
7.3 Safety and Complication Rates: Soft Tissue and Nerve Preservation The selective cutting mechanism of Piezosurgery provides a superior safety profile, particularly in anatomically challenging areas. Traditional drills are difficult to control with precision and can easily damage adjacent soft tissues if the clinician's hand slips. Piezosurgery's ultrasonic vibrations, however, do not harm soft tissues, thereby protecting vital structures such as nerves, arteries, and the delicate sinus membrane. This is of paramount importance during the extraction of lower wisdom teeth, where the inferior alveolar nerve is often in close proximity to the roots. Evidence suggests that Piezosurgery can reduce the risk of nerve damage by as much as 67% in these complex cases. The cavitation effect also contributes to safety by creating a clean, bloodless field, which improves visibility and reduces the risk of infection. 7.4 Bone Preservation and Healing Preserving the maximum amount of alveolar bone during an extraction is a critical long-term goal, especially if the patient plans to replace the tooth with a dental implant. Conventional extraction techniques, particularly those involving aggressive use of drills, can result in significant collateral bone loss, compromising the site for future restoration. Piezosurgery, with its precise and micrometric cutting, allows the surgeon to remove only the necessary amount of bone, preserving the architecture of the surrounding socket. This bone-sparing approach not only facilitates better healing but may also improve long-term outcomes for future implant placement. Furthermore, some research suggests that the ultrasonic vibrations may have a biostimulatory effect, potentially accelerating bone healing and regeneration by increasing the activity of bone-forming cells (osteoblasts). Table 3: Piezosurgery vs. Conventional Rotary Instruments: A Comparative Summary Clinical Parameter Piezosurgery Conventional Technique (Rotary Burs/Drills) Supporting Evidence Surgical Time Longer due to slower cutting speed. Significantly faster.
Post-Operative Pain Significantly reduced; minimal discomfort reported. Moderate to severe pain is common.
Post-Operative Swelling Minimal; reduced inflammatory response. Moderate to significant swelling is expected.
Risk of Nerve/Soft Tissue Injury Very low; selectively cuts hard tissue, preserving nerves, arteries, and membranes. Higher risk due to non-selective cutting action of rotary instruments.
Intraoperative Bleeding Minimal; cavitation effect creates a clean, visible surgical field. Can be significant, potentially obscuring the surgeon's view.
Alveolar Bone Preservation Excellent; precise, micrometric cuts spare surrounding bone architecture. Potential for significant collateral bone loss, compromising future implant sites.
Patient Comfort High; less invasive procedure with minimal noise and vibration. Lower; associated with anxiety due to noise, vibration, and invasive nature.
Part VIII: Clinical Application: A Survey of Piezosurgery Providers in Cầu Giấy, Hanoi The theoretical and clinical advantages of Piezosurgery have translated into its adoption in dental practices worldwide, including in metropolitan centers like Hanoi, Vietnam. An analysis of the dental market in the Cầu Giấy district reveals that this advanced technology is not only available but is also being actively promoted as a key service offering. This indicates a competitive dental landscape where clinics are investing in superior technology to attract a discerning patient base that values comfort, safety, and a premium clinical experience. The marketing language employed by these clinics directly reflects the patient-centric benefits established in clinical research, focusing on alleviating the common fears associated with tooth extraction. 8.1 Overview of Identified Dental Clinics A survey of dental providers in the Cầu Giấy district of Hanoi identifies several clinics that explicitly advertise the use of Piezosurgery or Piezotome (a common brand name for the technology) for tooth extractions. These clinics cater to the local population and position themselves as providers of modern, high-technology dental care. Among the identified providers are:
- Nha Khoa LaVita
- Nha Khoa Athena
- Nha Khoa Viet Smile
- Nha Khoa Lạc Việt Intech
- Nha Khoa Gia Đình
- Nha Khoa Thành An
- Nha Khoa Phương Nam
- Nha Khoa Sydney
- Nha Khoa Quốc tế Alisa
The presence of numerous clinics offering this technology within a single district suggests a significant level of market penetration and patient demand for advanced surgical options. 8.2 Summary of Services and Technological Capabilities These clinics primarily promote Piezosurgery for extractions, with a strong emphasis on wisdom tooth removal, which is often a surgical procedure with higher associated risks and patient anxiety. Their patient-facing materials explain that the technology uses ultrasonic waves to precisely and gently sever the periodontal ligaments that hold the tooth in place, allowing for its removal without significant trauma to the surrounding hard and soft tissues. Clinics like Nha Khoa Athena and Nha Khoa Viet Smile position the Piezotome method as a modern, superior alternative that overcomes the limitations and discomfort of traditional extraction techniques. The technology is presented as a cornerstone of their commitment to providing high-quality, minimally invasive care. 8.3 Analysis of Patient-Facing Information and Stated Benefits The marketing and informational materials from these Cầu Giấy clinics consistently highlight a core set of benefits that align directly with the clinical advantages of Piezosurgery. The language used is carefully chosen to address the primary concerns of dental patients: pain, fear, and recovery time. Commonly promoted benefits include:
- Painless and Gentle Procedure: Phrases such as "nhổ răng không đau" (painless tooth extraction), "nhẹ nhàng" (gentle), and "êm ái" (comfortable/smooth) are ubiquitous.
- Enhanced Safety: The ability of the technology to avoid damage to soft tissues, nerves, and blood vessels is a key selling point, promising a procedure with fewer complications.
- Reduced Trauma and Faster Healing: Clinics emphasize that the procedure minimizes trauma to the gums and jawbone, leading to less post-operative swelling and pain, and a faster overall recovery ("mau lành vết thương").
- Efficiency: Some clinics also claim that the procedure is faster than traditional methods, with Nha Khoa Athena, for example, advertising an extraction time of just 10-15 minutes for many cases.
This analysis demonstrates that the clinical value proposition of Piezosurgery—safer, less painful, and with a better recovery—is the central message being communicated to prospective patients in this competitive urban market. Table 4: Directory of Piezosurgery Providers in Cầu Giấy, Hanoi Clinic Name Address(es) Contact Information Advertised Technology Key Stated Benefits Nha Khoa Athena 97 Nghĩa Tân, Cầu Giấy 0988 622 606 Piezotome Ultrasound Painless, fast (10-15 mins), rapid healing, no complications Nha Khoa Viet Smile 70 Trần Thái Tông, Cầu Giấy 1900 3331 Piezosurgery Gentle, fast, limits soft tissue damage, safe, promotes rapid healing Nha Khoa LaVita Tầng 1, 34T Hoàng Đạo Thuý, Trung Hoà, Cầu Giấy 0904 721 122 Piezo-Ultrasonic / Piezotome Reduces post-operative pain, supports wound healing, preserves alveolar bone Nha Khoa Lạc Việt Intech 9 Nguyễn Văn Huyên, Cầu Giấy 0971 066 726 (Service offered) Provides painless wisdom tooth extraction services Nha Khoa Gia Đình 3 Nguyễn Ngọc Vũ, Cầu Giấy; 16 Trần Thái Tông, Cầu Giấy 1900 0058 (Service offered) Provides wisdom tooth extraction services Nha Khoa Quốc tế Alisa 33 Nguyễn Phong Sắc, Cầu Giấy 024 3371 7777 (Service offered) Provides aesthetic, safe, and painless wisdom tooth extractions Nha Khoa Phương Nam 36 Hồ Tùng Mậu, Cầu Giấy 0941 944 977 (Service offered) Provides wisdom tooth extraction services Part IX: Concluding Analysis and Patient Recommendations This clinical review has provided a comprehensive examination of dental extraction, from its foundational indications to the procedural nuances and the impact of advanced surgical technologies. The analysis reveals a procedure that has evolved significantly from a simple remedy for a painful tooth into a sophisticated and strategic intervention integral to comprehensive oral and systemic health management. 9.1 Synthesis of Findings: The Evolving Standard of Care The decision to extract a tooth is multifaceted, driven by pathology, trauma, developmental needs, and even prophylactic systemic health concerns. The procedure itself is clearly stratified into simple and surgical categories, a distinction that fundamentally dictates the entire clinical pathway, including the required expertise, anesthesia level, cost, and recovery profile. Post-operative care is not a passive phase but an active partnership between the clinician and patient, with patient compliance being a critical factor in preventing common complications like alveolar osteitis. The protocols for post-operative management are physiologically grounded, with nearly every instruction aimed at the singular goal of protecting the vital blood clot. The advent of Piezosurgery marks a significant technological leap in oral surgery. The evidence strongly supports its clinical benefits, demonstrating that its use leads to reduced post-operative pain, swelling, and trismus, a superior safety profile with minimal risk to soft tissues and nerves, and better preservation of alveolar bone. These advantages, however, come at the cost of longer surgical times and higher equipment expense. This establishes a clear clinical trade-off between procedural efficiency and the quality of the patient outcome. The widespread adoption and marketing of this technology, as seen in the Cầu Giấy, Hanoi market, indicate a shift in patient priorities toward comfort, safety, and minimally invasive care. 9.2 Informed Decision-Making: A Framework for Patients Patients facing a dental extraction can and should be active participants in their care. An informed patient is better equipped to understand their treatment plan, manage their expectations, and contribute to a successful outcome. It is recommended that patients discuss the following key questions with their dentist or oral surgeon: 1. Procedural Classification: "Is my extraction considered simple or surgical, and what specific factors in my case lead to that classification?" 2. Anatomical Risks: "Are there any specific risks associated with my extraction, such as the tooth's proximity to a nerve or the maxillary sinus? How will these risks be managed?" 3. Anesthesia and Sedation: "What are my options for anesthesia and sedation? Based on the complexity of the procedure and my personal anxiety level, what would you recommend to ensure my comfort?" 4. Technology and Technique: "What technique will be used for my extraction (conventional or Piezosurgery)? If Piezosurgery is an option, would it be clinically beneficial for my specific case, and what are the associated costs?" 5. Post-Operative Expectations: "What should I expect during recovery in terms of pain, swelling, and dietary restrictions? What are the key signs of a complication, like dry socket, that I should watch for?" 9.3 Future Outlook: Emerging Technologies and Trends in Oral Surgery The field of oral surgery continues to advance, driven by the demand for procedures that are ever more precise, less invasive, and conducive to faster healing. While Piezosurgery represents the current state-of-the-art for atraumatic bone surgery, it is part of a broader trend. Emerging technologies such as laser-assisted extraction promise further benefits, including minimal bleeding due to the cauterizing effect of the laser and sterilization of the surgical site, which may lower infection risk and accelerate healing. Looking further ahead, the integration of digital technologies will continue to transform the field. Trends may include the use of artificial intelligence (AI) to modulate laser energy for enhanced precision or the incorporation of robotic guidance systems to assist surgeons in performing procedures with unparalleled accuracy. These innovations signal a future where surgical interventions are increasingly technology-driven, further minimizing trauma, improving predictability, and continuing to elevate the standard of care to prioritize patient safety and quality of life. Works cited 1. Tooth Extraction: Surgery & Healing – Cleveland Clinic, https://my.clevelandclinic.org/health/treatments/22120-tooth-extraction 2. 8 Reasons for Tooth Extraction – Total Dental Care Blog, https://www.drtonylee.com/blog/8-reasons-for-tooth-extraction/ 3. Five Common Reasons for Tooth Extraction – Oral & Facial Surgeons of Arizona, https://www.oralsurgeryarizona.com/five-common-reasons-tooth-extraction/ 4. Reasons for Tooth Extraction | Manhattan, KS, Best Dentists Near You, https://www.downtowndentalmanhattan.com/manhattan-ks/services/general-dentistry/tooth-extractions/reasons/ 5. Types of Dental Extractions | Tooth Extraction and Removal – Hamlin Modern Dentistry, https://www.hamlinmoderndentistry.com/blog/types-of-dental-extractions.html 6. What's The Difference Between A Simple Extraction And A Surgical Extraction? – Wellesley Dental Arts, https://www.wellesleydentist.com/whats-the-difference-between-a-simple-extraction-and-a-surgical-extraction/ 7. What's the Difference Between Oral Surgery & Tooth Extractions? – Bellevue Dental Oasis, https://bellevuedentaloasis.com/blog/oral-surgery-vs-tooth-extractions/ 8. Tooth Extraction from Start to Finish – Century Dental, https://www.centurysmiles.com/blog/tooth-extraction-start-finish/45134 9. Dental Corner: How to perform a surgical extraction – DVM360, https://www.dvm360.com/view/dental-corner-how-perform-surgical-extraction 10. Types of Dental Extraction – News-Medical, https://www.news-medical.net/health/Types-of-Dental-Extraction.aspx 11. Step-by-Step Process of Tooth Extraction: How Dentists Extract a Tooth – Simply Dental Chatswood, https://www.simplydentalchatswood.com.au/tooth-extraction-explained-step-by-step/ 12. A Step-by-step Guide to a Tooth Extraction Procedure – Lasting Impressions Dental Group Houston TX, https://www.lastingimpressionsdentalgroup.com/blog/a-step-by-step-guide-to-a-tooth-extraction-procedure/ 13. Anesthesia | UT Dentistry – UT Health San Antonio, https://uthscsa.edu/utdentistry/services/anesthesia 14. What Kind of Sedation Is Used for Tooth Extraction? A Comprehensive Guide – Emmy Dental, https://www.emmydental.net/what-kind-of-sedation-is-used-for-tooth-extraction/ 15. 3 Types of Anesthesia Used During Oral Surgery | OMSNashville TN, https://omsnashville.com/blog/oral-health/3-types-of-anesthesia-used-during-oral-surgery/ 16. Anesthesia | Sedation Options for Oral Surgery, https://havemeyeroms.com/procedures/anesthesia/ 17. General Post-Operative Instructions – Canyon Oral & Facial Surgery, https://www.canyonofs.com/post-operative-instructions/ 18. Dry socket – symptoms, treatments and causes – Healthdirect, https://www.healthdirect.gov.au/dry-socket 19. Teeth Extractions | Oral and Maxillofacial Surgery – McGill University, https://www.mcgill.ca/omfs/patient-info/teeth-extractions 20. Post-Operative Instructions: General – The Oral Surgery & Dental Implant Specialists of San Diego, https://www.sandiegooralsurgery.com/post-operative-instructions/ 21. Post-Procedure & Dental Care Instructions – Harvard School of Dental Medicine, https://www.hsdm.harvard.edu/post-procedure-dental-care-instructions 22. Dry socket – Symptoms and causes – Mayo Clinic, https://www.mayoclinic.org/diseases-conditions/dry-socket/symptoms-causes/syc-20354376 23. Tooth Extraction Complications: Risks To Watch For, https://naidudental.com/tooth-extraction-complications/ 24. Nerve Pain After Tooth Extraction: Causes and Solutions – BLVD Dentistry & Orthodontics, https://www.blvddentistry.com/managing-nerve-pain-after-tooth-extraction-a-guide/ 25. Piezosurgery Boca Raton FL | Ultrasound Gum Treatment, https://www.surgicalartsofbocaraton.com/procedures/piezosurgery/ 26. Piezosurgery: A Boon for Modern Periodontics – PMC, https://pmc.ncbi.nlm.nih.gov/articles/PMC5343677/ 27. The Top 4 Benefits of PIEZOSURGERY® | Amalfitano Center for …, https://www.michiganimplantcenter.com/the-top-4-benefits-of-piezosurgery/ 28. What Is Piezosurgery? | Bone Surgery – Clarity Dental Center, https://www.federalwayimplantlaser.com/blog/what-is-piezosurgery.html 29. Piezosurgery vs Laser Extraction: 5 Key Differences to Know, https://drmaniarash.com/en/piezosurgery-vs-laser-extraction-wisdom-teeth/ 30. Piezo Non Invasive Extractions Lawndale CA – Vadadent Modern Dental Group, https://www.digitaldentistryclinic.com/treatments/piezo-non-invasive-extractions/ 31. 5 Reasons We Use Piezosurgery | Flushing Oral Surgery & Dental …, https://flushingoms.com/5-reasons-we-use-piezosurgery/ 32. Máy phẫu thuật siêu âm PIEZOSURGERY® touch – Công ty TNHH Nha khoa Thái Bình Dương, https://thaibinhduongdental.com/may-phau-thuat-sieu-am-piezosurgery-touch 33. Piezosurgery: A Look at the Top Five Reasons for Jaw Surgery, https://www.niguelcoastoralsurgery.com/five-reasons-for-jaw-surgery/ 34. Piezosurgery in Third Molar Extractions: A Systematic Review – MDPI, https://www.mdpi.com/2075-4426/14/12/1158 35. NHỔ RĂNG KHÔN NHẸ NHÀNG ÊM ÁI VỚI CÔNG NGHỆ …, https://nhakhoaduchau.vn/nho-rang-khon-nhe-nhang-em-ai-voi-cong-nghe-piezotome/ 36. Địa chỉ nhổ răng khôn uy tín ở Cầu Giấy bằng máy piezotome – Viện …, https://nhakhoaathena.vn/dia-chi-nho-rang-khon-uy-tin-o-cau-giay-bang-may-piezotome/ 37. Nhổ răng khôn công nghệ cao bằng máy siêu âm Piezotome, https://nhakhoalavita.com.vn/nho-rang-khon-cong-nghe-cao-bang-may-sieu-am-piezotome-1 38. Top phòng Khám Nha Khoa Cầu Giấy Hà Nội Uy Tín, Giá Tốt 2024, https://nhakhoathanhan.vn/phong-kham-nha-khoa-cau-giay/ 39. Top 5 phòng khám nha khoa uy tín tại Hà Nội, Cầu Giấy, https://nhakhoaathena.vn/phong-kham-nha-khoa-uy-tin-nhat-tai-ha-noi/ 40. So sánh công nghệ nhổ răng Piezosurgery với phương pháp truyền thống – YouTube, https://www.youtube.com/watch?v=2PA0O_kFRyE 41. NƠI GỬI TRỌN NIỀM TIN SỨC KHỎE RĂNG MIỆNG – NHA KHOA VIET SMILE, https://nhakhoavietsmile.com/gioi-thieu-ve-nha-khoa-viet-smile/ 42. Top 10+ Phòng Khám Nha Khoa Cầu Giấy Chất Lượng Nhất – ViDental Clinic, https://videntalclinic.com/phong-kham-nha-khoa-cau-giay-6378.html 43. 13 Địa chỉ nhổ răng khôn tại Hà Nội uy tín và giá rẻ nhất hiện nay – Nha khoa Parkway, https://nhakhoaparkway.com/dia-chi-nho-rang-khon-tai-ha-noi/ 44. Top 10 địa chỉ trồng răng Implant Hà Nội uy tín 2025 – Nha khoa Parkway, https://nhakhoaparkway.com/dia-chi-trong-rang-implant-tai-ha-noi/ 45. Trồng răng implant Cầu Giấy Hà Nội – Nha khoa Alisa, https://alisadental.com/nha-khoa-alisa-trong-rang-implant-cau-giay-ha-noi/